A doctor's dream
The faces behind the development
of a new drug for sleeping sickness
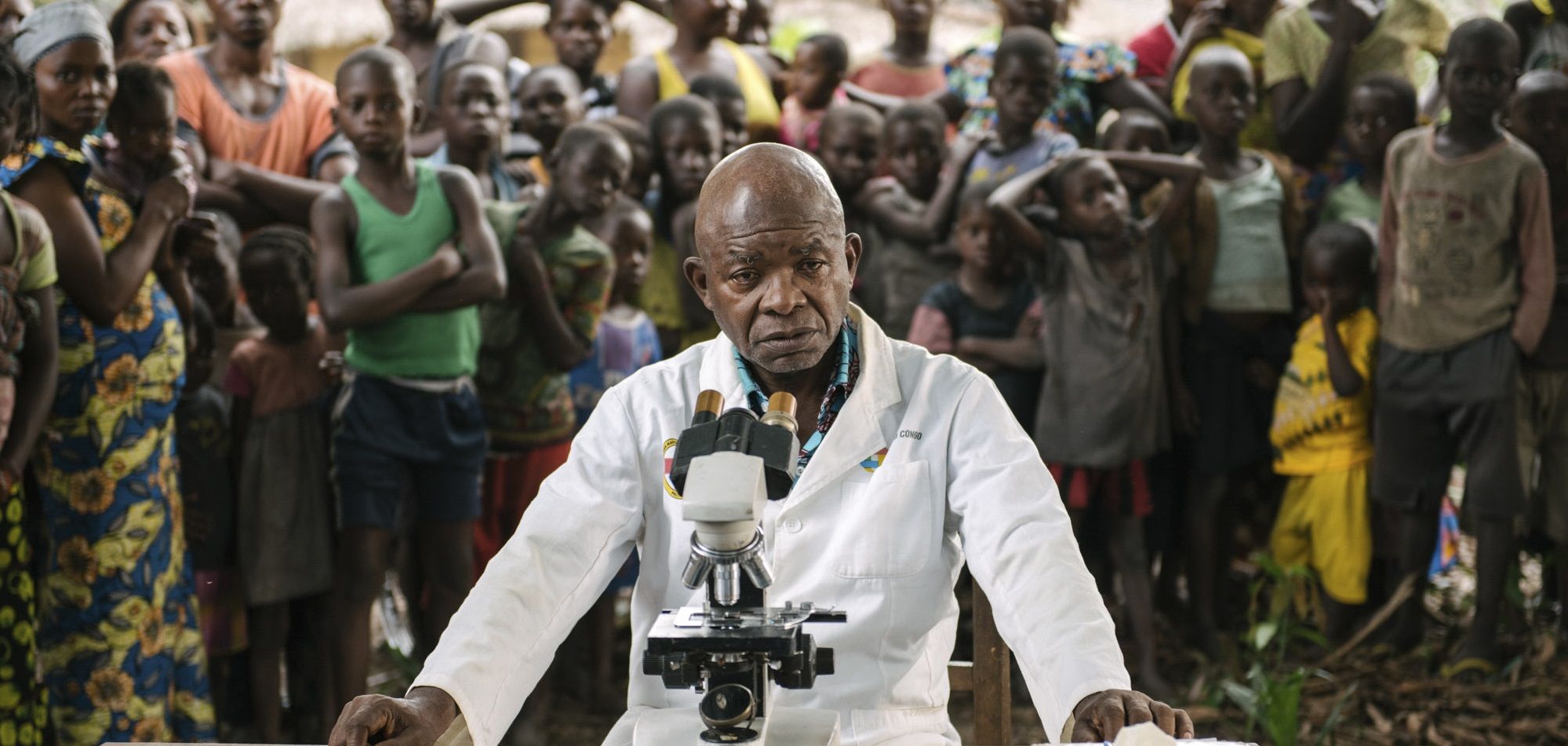
For decades doctors in the Democratic Republic of Congo have dreamed of better sleeping sickness treatments for patients living in remote areas

Fexinidazole, the first all-oral drug for both stages of sleeping sickness was approved in November 2018
Here are the stories of the doctors, patients, and scientists who contributed to this story:

16 November 2018
Alexis Mukwedi sits on a wooden chair under a large shady tree in Lwano village, his bloodshot eyes filled with fear. A mobile team of health workers had arrived the day before at this remote village, carting microscopes, generators, diagnostic machines, and other material through the deep bush of Bandundu province in the Democratic Republic of Congo (DRC).
After a number of blood tests he was diagnosed earlier that morning with a deadly disease that is synonymous with fear in his country – sleeping sickness. The young father and fisherman had felt ill for a while now – he was feverish, sleeping during the day, up at night and complained of nervous tics.
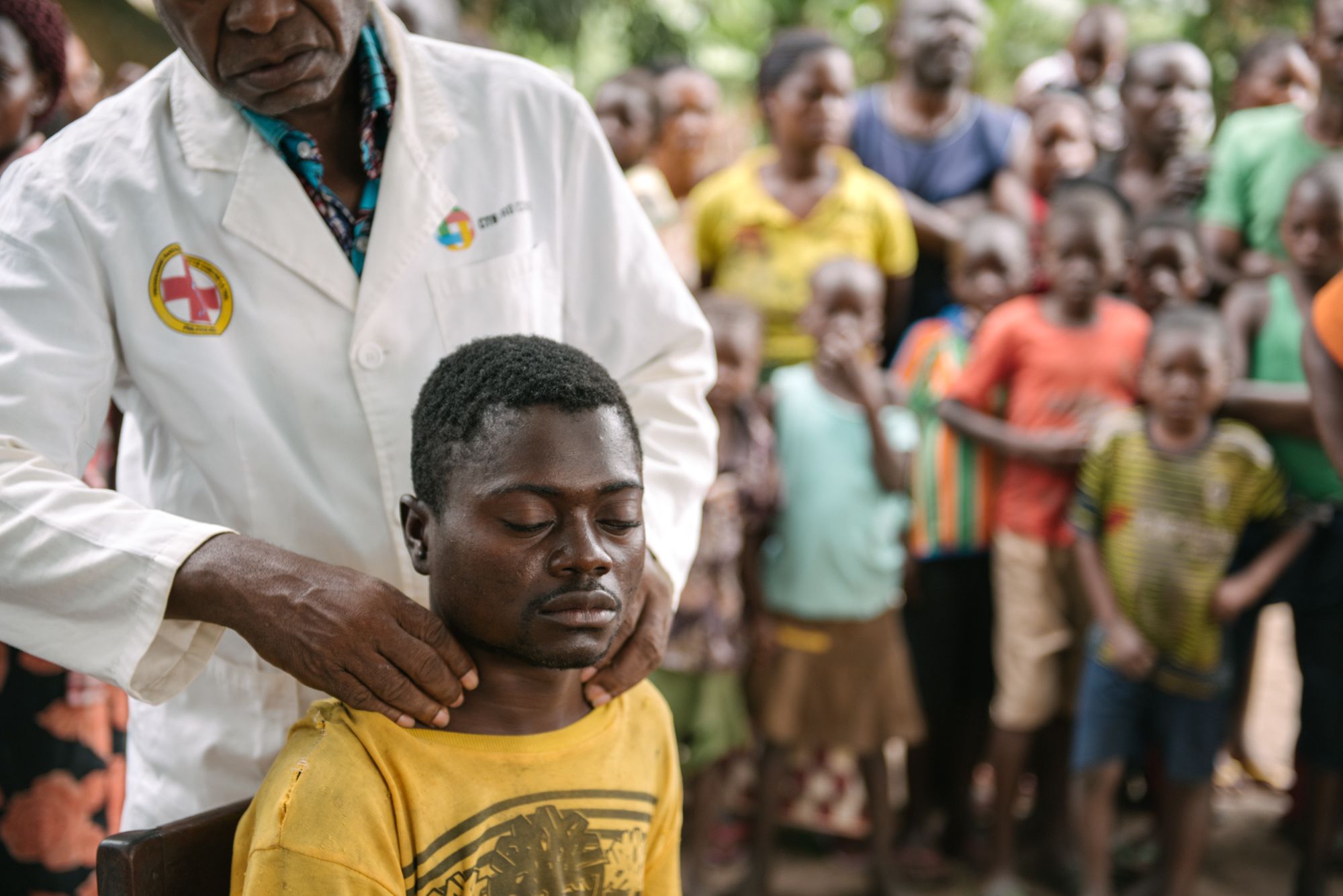
Dr Kande examines Alexis
Dr Kande examines Alexis
Behind Alexis, an elderly doctor expertly examined his swollen lymph nodes, looking for a tell-tale clinical sign of the disease. After a few moments the doctor – who has clearly done this thousands of times before – nodded slowly as he walked away. “C’est la maladie du sommeil,” said the older man, Dr Victor Kande.
Indeed, Dr Kande had done this exam countless times before. He has treated thousands of sleeping sickness patients throughout his long career– from his time as a local doctor in the remote Equateur region of the DRC – up until his tenure as head of the DRC’s National Sleeping Sickness Programme. Now he is the principal investigator of a clinical trial for a drug known as fexinidazole, an improved sleeping sickness treatment that is all-oral and can be given over 10 days as a course of pills. It is a treatment that he has dreamed about for decades.

Dr Kande crosses the river Kwilu to Bagata hospital
Dr Kande crosses the river Kwilu to Bagata hospital
The mobile team came from neighbouring Bagata hospital, one of the sites for this clinical trial. After Alexis tested positive the health workers asked if Alexis wanted to be enrolled in a trial. He agreed.
“He’s scared,” said Dr Kande as health workers prepared Alexis for the trip to Bagata. “People are frightened of this disease, but they are also scared of the treatments.”
Why? For decades the only treatment available for sleeping sickness was based on arsenic, killing 1 in 20 patients. And newer treatments are safe but involve a long hospital stay with multiple injections.
But Alexis will receive fexinidazole as part of a clinical trial, a treatment that should change the course of how this disease is treated. Note: Fexinidazole was approved in November 2018 and registered in the DRC in December 2018.
See how doctor Kande's dream become a reality:
Fexinidazole is the success of hundreds of people from diverse backgrounds, involving scientists working for the Drugs for Neglected Diseases initiative (DNDi), the not-for-profit research and development (R&D) organization that led trials for the treatment in Africa. It involved researchers from Sanofi, the pharmaceutical company that partnered with DNDi to develop its drug. Finally, the success would never have happened without the frontline health workers in DRC, and the patients who agreed to take part in the clinical trial.
But our story starts with the“tsetse” fly. They can bite near the rivers, lakes, and marshes that dot the Democratic Republic of Congo, where around 80% of sleeping sickness cases are found.
And so the journey begins on the riverbank…

Currently about 65 million people are at risk of sleeping sickness in rural areas of sub-Saharan Africa. After the tsetse fly takes a blood meal and transmits the parasite that causes sleeping sickness, people experience fever and chills – symptoms that are often mistaken for malaria.
Patients enter the second, deadly stage of the disease when the parasites cross over into the central nervous system. Patients then suffer from terrifying neuropsychiatric symptoms, including aggression, psychosis, and a debilitating disruption of sleep patterns. Without treatment, most patients will die.
Historical accounts of the DRC are full of lurid descriptions of sleeping sickness and its symptoms. Colonial records talk about entire regions emptied out because of tsetse flies. Local village legends talk of sorcery and black magic, because the disease leads to such dramatic changes in the behaviour of their loved ones.
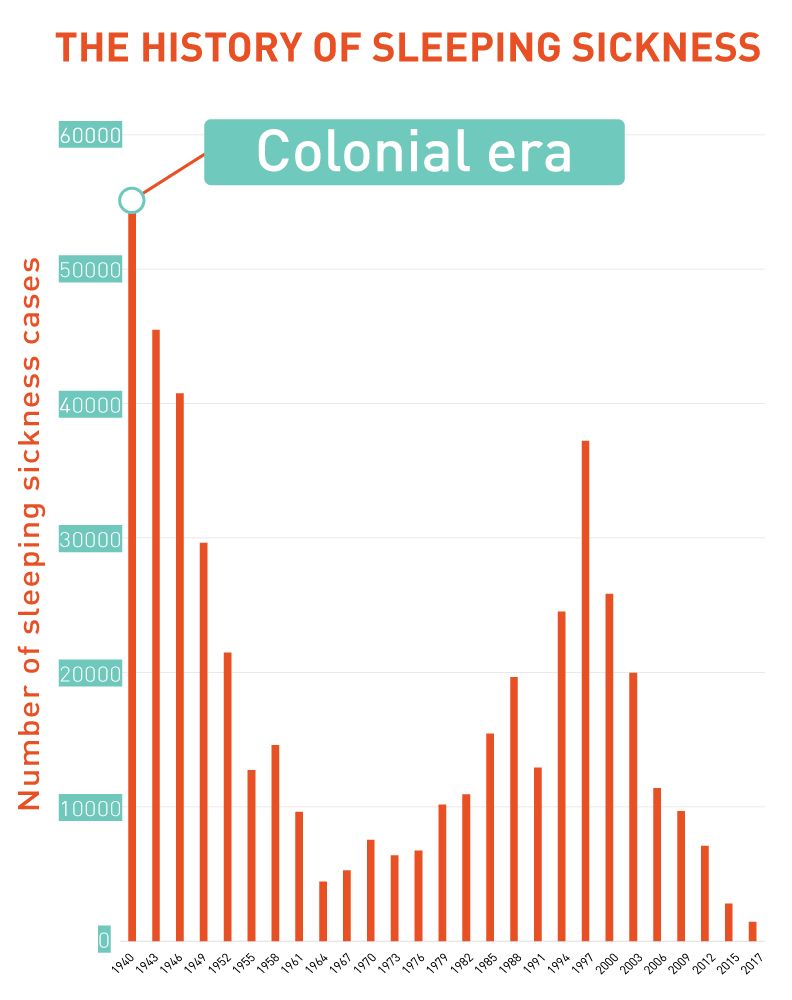
While records exist of sleeping sickness in early African civilizations, the violent changes brought on by colonialism sparked the first large-scale outbreaks at the end of the 19th century. Up to 500,000 died in one outbreak in the Belgian Congo in the 1890s, and 200,000 in British-controlled Uganda died from sleeping sickness.
In response, colonial authorities in the most hard-hit countries began long-term campaigns to eliminate the disease. European researchers crisscrossed the Congo while French “mobile teams” penetrated deep into the forests of Cameroon, pioneering the “Jamot Method” of case detection and treatment.
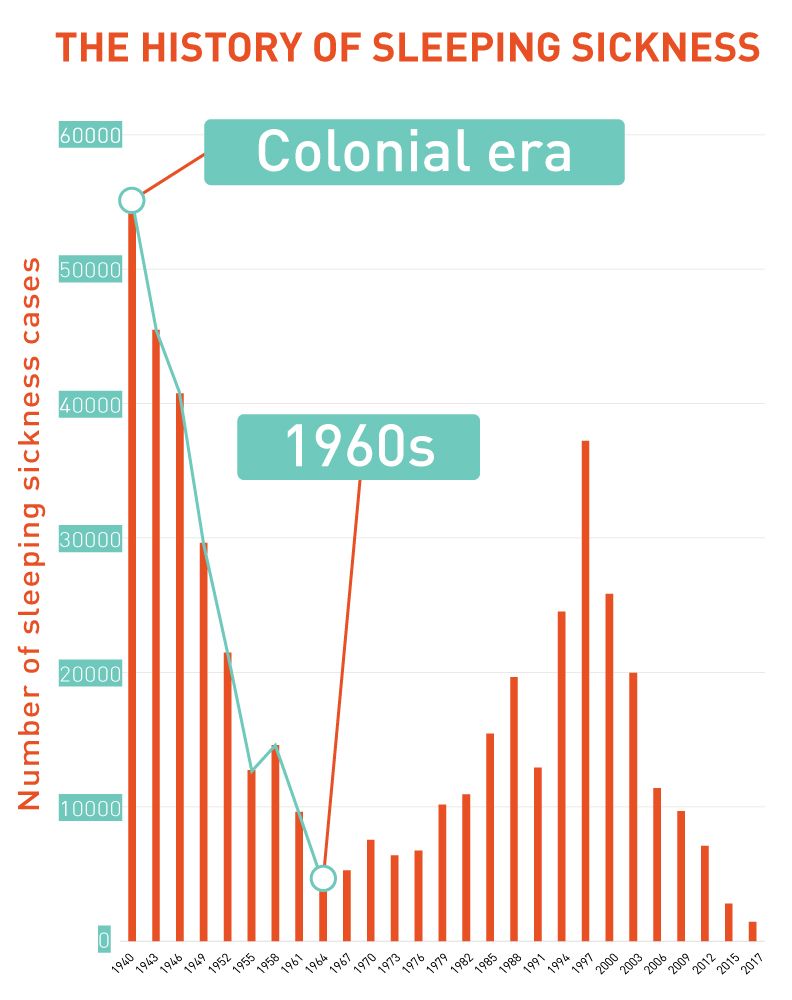
By the 1960s this approach succeeded in reducing the number of cases to below 5,000 per year. But independence led to the end of international aid. A lack of resources meant greatly reduced screening and tsetse fly control. Sleeping sickness cases began to come back.
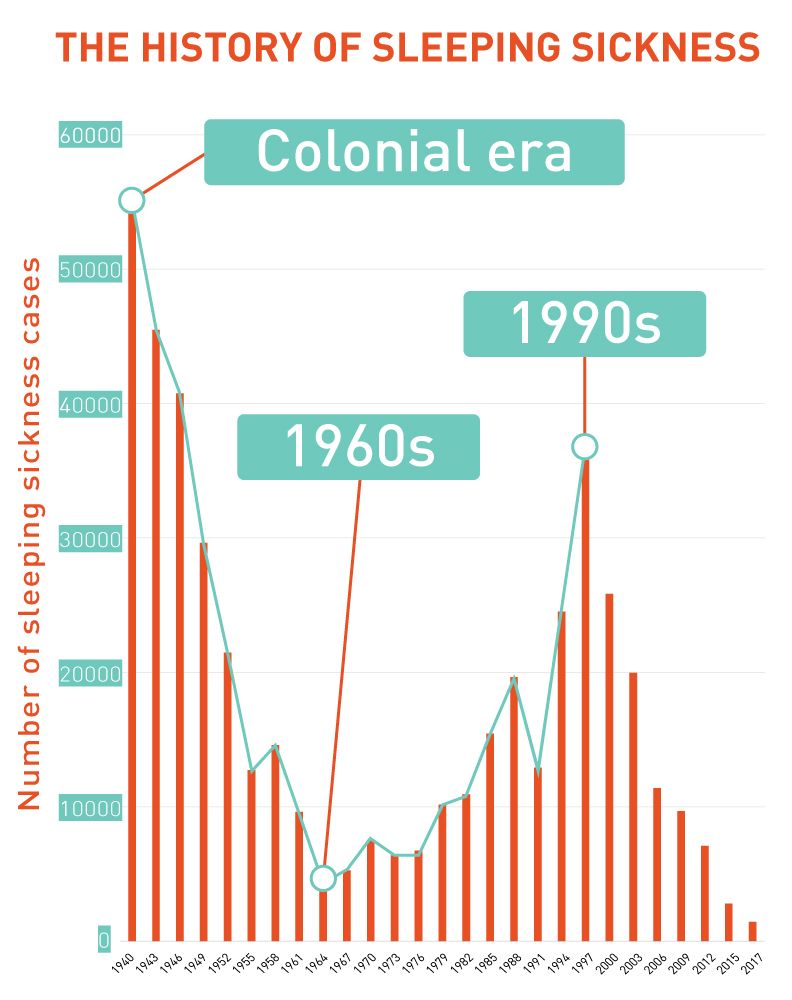
The 1990s saw increased war and conflict in Sudan and the DRC. After years of neglect since the 1960s, sleeping sickness epidemics broke out in these countries, made worse by massive population displacement, poverty and violence.
By the 2000s the global community stepped up. The World Health Organization (WHO) signed donation agreements with pharmaceutical companies such as Aventis (later Sanofi) and Bayer to access treatments and control the disease. International aid began to flow again. The number of reported cases dropped below 10,000 for the first time in decades. By 2017, only 1447 cases were reported to the WHO.
Excitement is now growing that elimination of sleeping sickness is in sight.
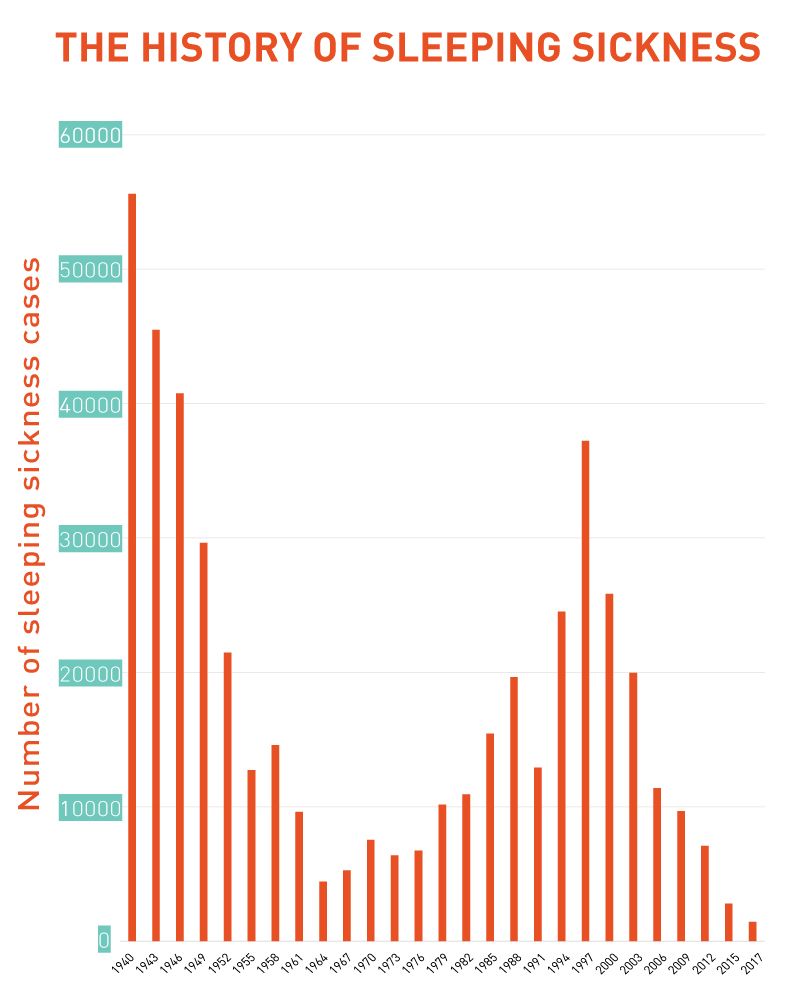
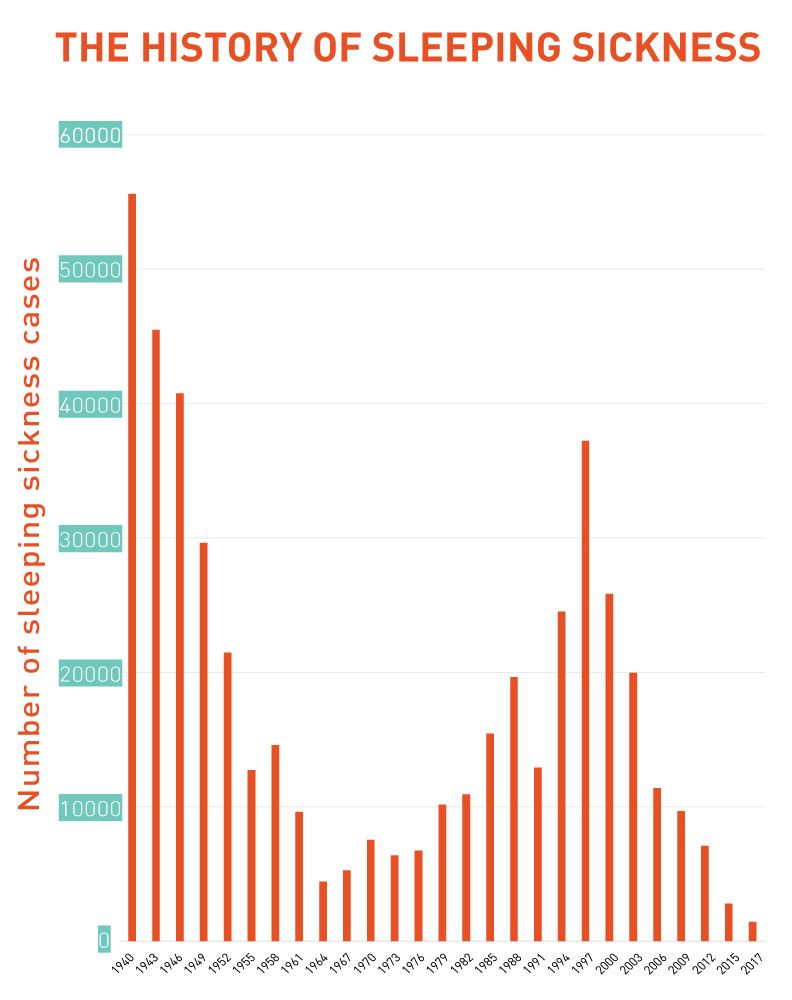
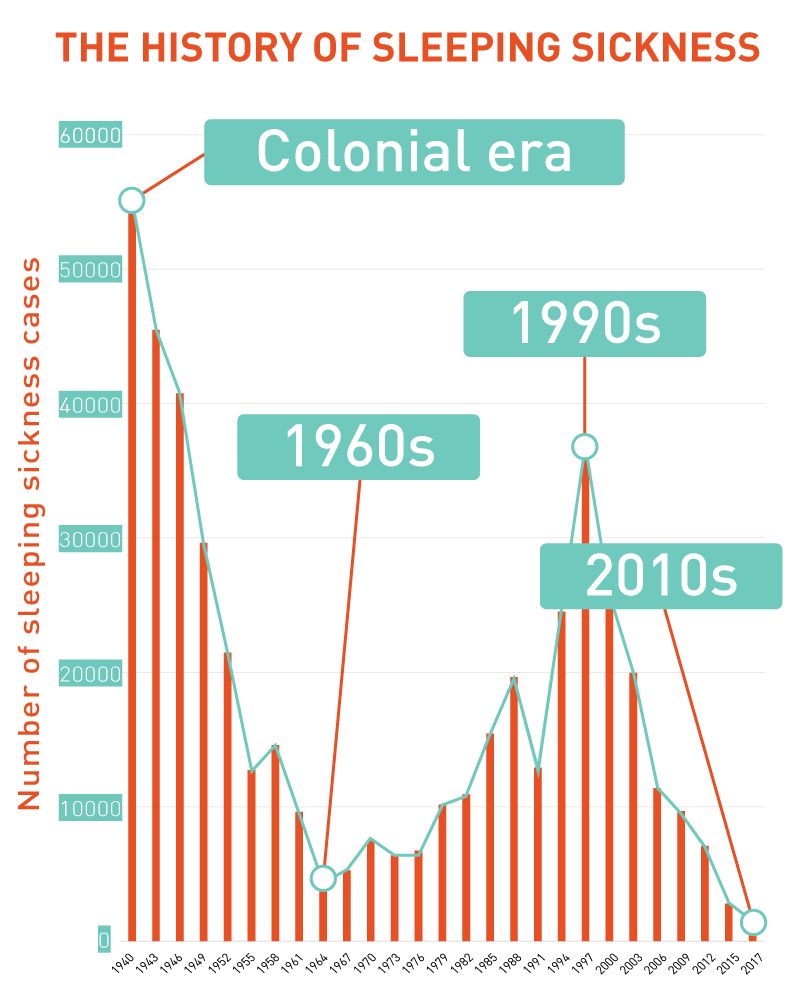
From nightmare to a dream - the evolution of sleeping sickness treatment
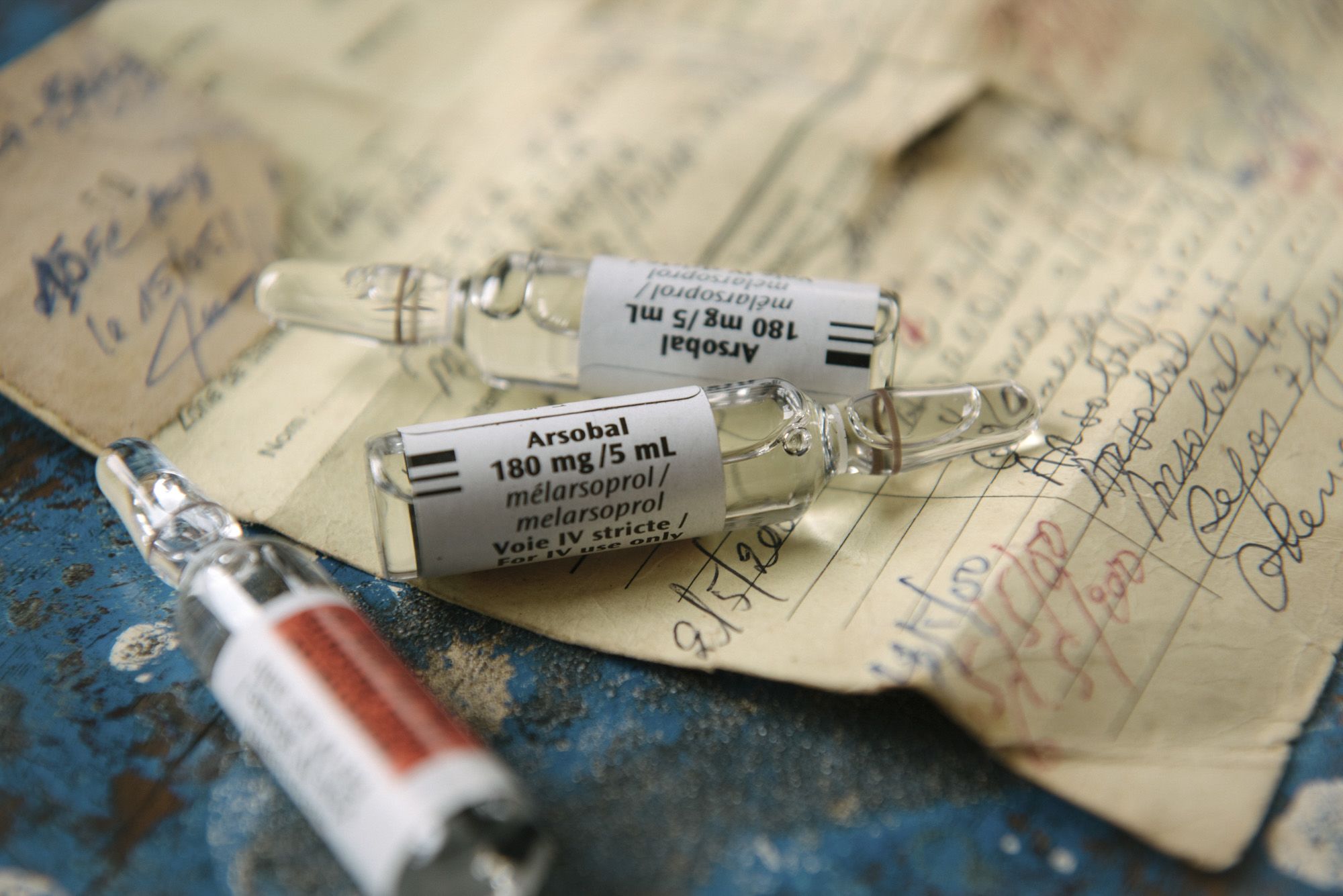
Nothing sums up the frustrations of sleeping sickness doctors more than the feared arsenic-based treatment melarsoprol (sometimes better known under its brand name Arsobal).
Discovered in the 1940s, melarsoprol killed 1 in 20 patients due to its toxicity. If the treatment touched bare skin it caused severe burns, sometimes leading to amputations.
Doctors recall that patients would scream as the arsenic-based treatment was injected. Because of the fear of side effects or even death, patients would avoid going to the hospital for treatment, even after they were diagnosed with sleeping sickness.

Madeleine Mouzela Kafuti received melarsoprol in 2000. "I was scared," she remembers. "I knew many people died from this treatment"
Madeleine Mouzela Kafuti received melarsoprol in 2000. "I was scared," she remembers. "I knew many people died from this treatment"
It was this unimaginable situation that led doctors from Médecins Sans Frontières/Doctors without Borders (MSF) to call for the creation of DNDi in the early 2000s. MSF had been on the frontline of sleeping sickness outbreaks in the 1990s, and doctors returning from the field brought horror stories of these toxic treatments.
Action needed to be taken.

"It felt like fire and my veins turned black," Dieudonné Likilo Taetae, who received melarsoprol in 2003
"It felt like fire and my veins turned black," Dieudonné Likilo Taetae, who received melarsoprol in 2003
After his wife died of sleeping sickness in 2003, Jean Osombindeliye (pictured under the net) travelled 35 km on a bike with his two children to the MSF clinic in Isangi on the Congo river. His two kids were sleeping all day and he was scared.

The bike Jean used to transport his children to the MSF clinic
Jean Osombindeliye at home
Both his children received treatment and were cured, but one child, Dominique, still to this day suffers from neurological symptoms – wandering around the village, not able to attend school. Doctors attribute this to melarsoprol or the long-term effects of sleeping sickness – or both.
Isangi eventually became an important site for a clinical trial run by MSF and DNDi for a new treatment called NECT, which combined the drugs eflornithine and nifurtimox. Dominique eventually got a job at the site, working as a security guard. NECT was approved in 2009, and finally led to the replacement of melarsoprol in the country. Doctors call it “the first revolution in treatment.”
But NECT wasn’t exactly the dream Dr Kande and other Congolese doctors had hoped for. While it is extremely effective for the second stage of sleeping sickness, NECT is difficult to ship, store and administer.

Large cumbersome boxes of NECT need to be shipped from Kinshasa to remote corners of the DRC – often taking a journey from a boat, up a river bank and into remote locations. Patients must stay in the hospital for ten days to receive the daily intravenous infusions.
An oral, easy-to-take treatment was needed, especially for the second stage of the disease.



On the frontlines of clinical research
Masi Manimba
Isangi wasn’t the only remote site for sleeping sickness research in Congo. A number of hospitals, once places where people suffered from toxic treatments, became centres for clinical research – an almost improbable transformation. In order to run clinical trials in these areas, DNDi brought them up to international standards of clinical research, installing lab equipment, solar panels, refurbishing clinics– even setting up an internet connection.
One DNDi site is so associated with sleeping sickness that the town it is located in is named after the disease.

Masi Manimba, located in the Bandundu region, means “the place where people sleep” in the local Kikongo language, and locals are sure that this is because of sleeping sickness. People are bitten by tsetse flies working in the fields or tending to their fish farms which are found in the rolling valleys of the region.
Lab technician Leon Katunda works at the DNDi ward at the Masi Manimba General Reference Hospital, which has become a flagship site for DNDi clinical trials in the country. He has worked in sleeping sickness for 16 years, starting off in the mobile teams that go out to remote villages to test for sleeping sickness.

Today Leon is enrolling two patients into DNDi clinical trials. They were brought to the trial site by the mobile teams, and sit in the spacious DNDi ward, located behind the hospital.
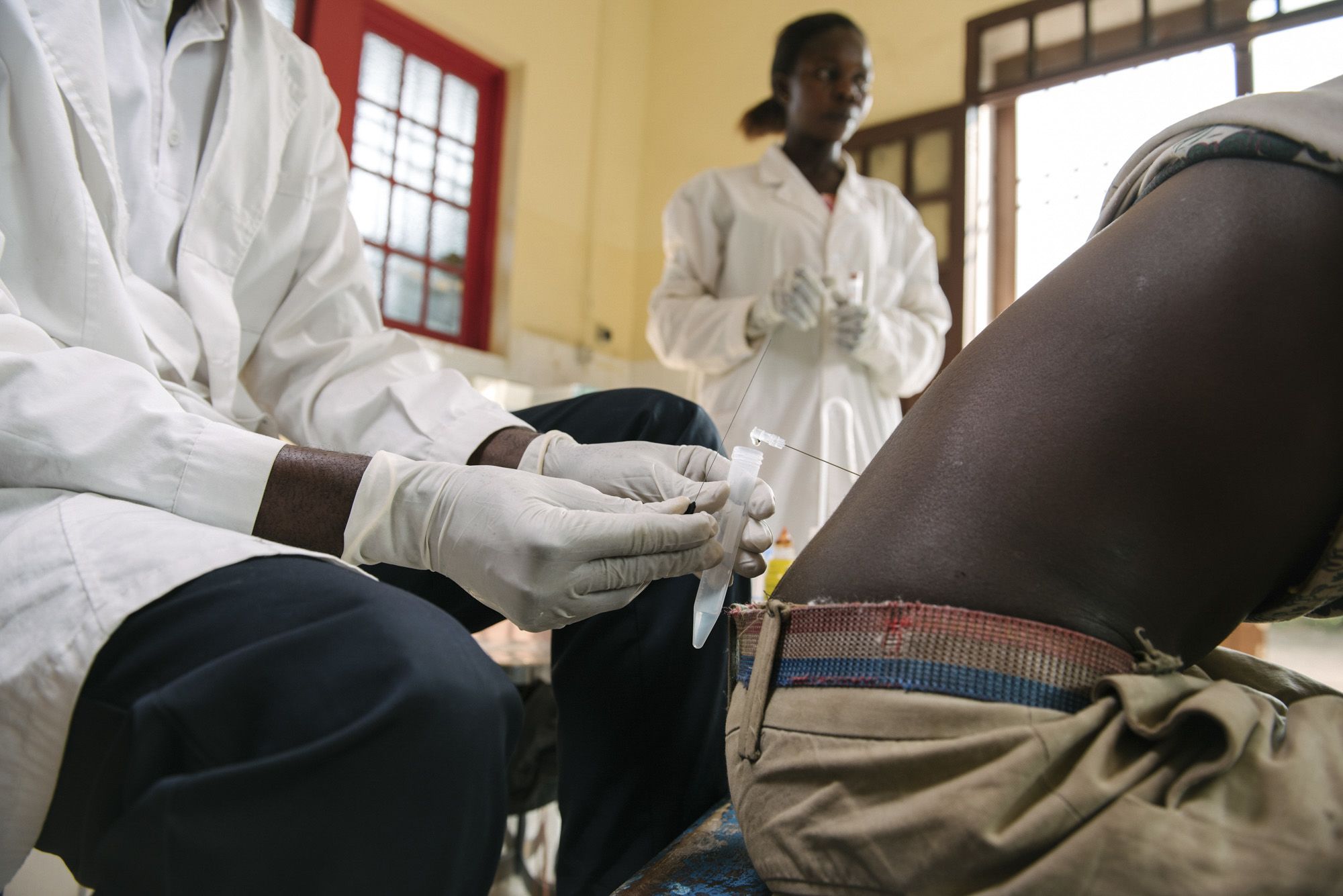
But first they must undergo another medical process that has become deeply associated with sleeping sickness: the spinal tap. To see if a patient has progressed to the second stage of sleeping sickness, doctors must extract their cerebrospinal fluid to check if parasites have entered the central nervous system. “We feel bad doing something that hurts our patients,” said Leon as he gently prepared a patient. “But we explain to the patients that without the lumbar punctures, we cannot treat them.”
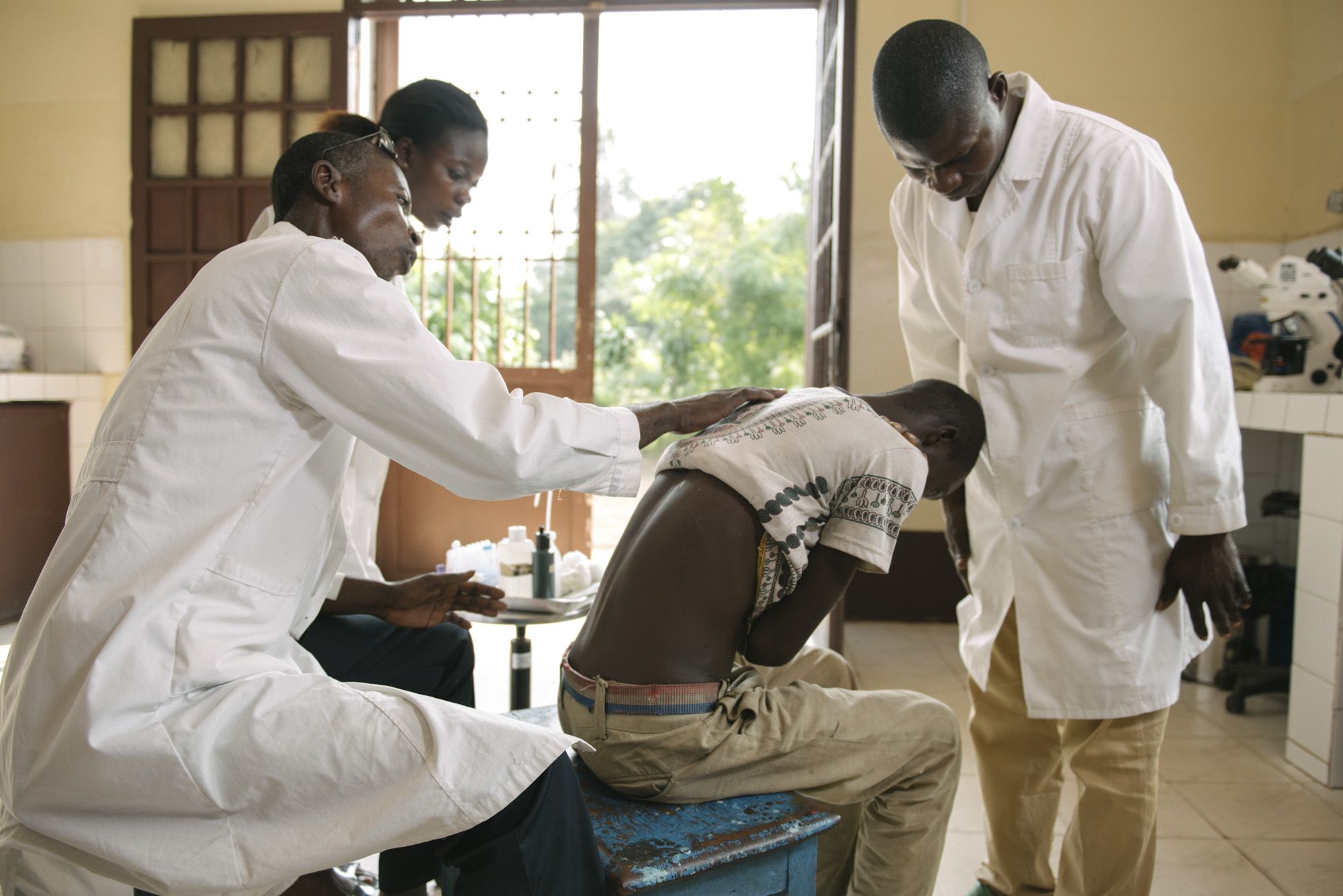
Both patients grimace as Leon expertly inserts a spinal tap into their lower back – without anaesthesia. But they are brave, showing almost little pain. Leon collects the fluid from the tap.
The samples are then analysed by the clinical team. Dr Willy Kuziena, Investigator for the trials at Masi Manimba, oversees the operation. The samples are examined under microscopes with the aid of specialized software and a tablet that can take photos. The imagery can then be sent using the site’s internet connection.
Dr Willy has dedicated years of his life to developing fexinidazole and he couldn’t be happier.
“Many patients don’t want to go to the hospital because they fear leaving their fields for too long,” he says. “Fexinidazole would be a huge improvement because we could treat patients in their health zones and nurses don’t need specialized training.”
This was the “second revolution” that doctors needed, after NECT.

Lab technician Georgine Kambela in the DNDi lab
In the DNDi lab at Masi Manimba

Lab technician Georgine Kambela in the DNDi lab
In the DNDi lab at Masi Manimba

Lab technician Leon Katunda
Lab technician Leon Katunda

Lab technician Leon Katunda
Lab technician Leon Katunda

Examining the samples
Examining the samples

Examining the samples
Examining the samples

Dr Willy Kuziena, investigator at Masi Manimba
Dr Willy Kuziena, investigator at Masi Manimba (left)
Bandundu
Bandundu Hospital hosts another DNDi site in the DRC, located in Bandundu on the Kwango river. Dr Hélène Mahenzi is the trial investigator and has been managing DNDi’s studies for six years. Around 160 people have been recruited by her team – she is proud of this achievement, especially in an area where clinical trials are unknown and capacity was limited.
Today she is examining a patient that wasn’t included in the trial. The patient, Jonathan Kidima is a student and is 24 years old. The DNDi ward admits other non-clinical patients as well. Because Jonathan is in the second stage, he will receive NECT – the standard of care at the time.
When night falls it is time to give Jonathan his nightly infusion. Sitting by Jonathan’s bedside is his mother, Mama Philomene. She brought her son to Bandundu hospital more than 60km away from their village.
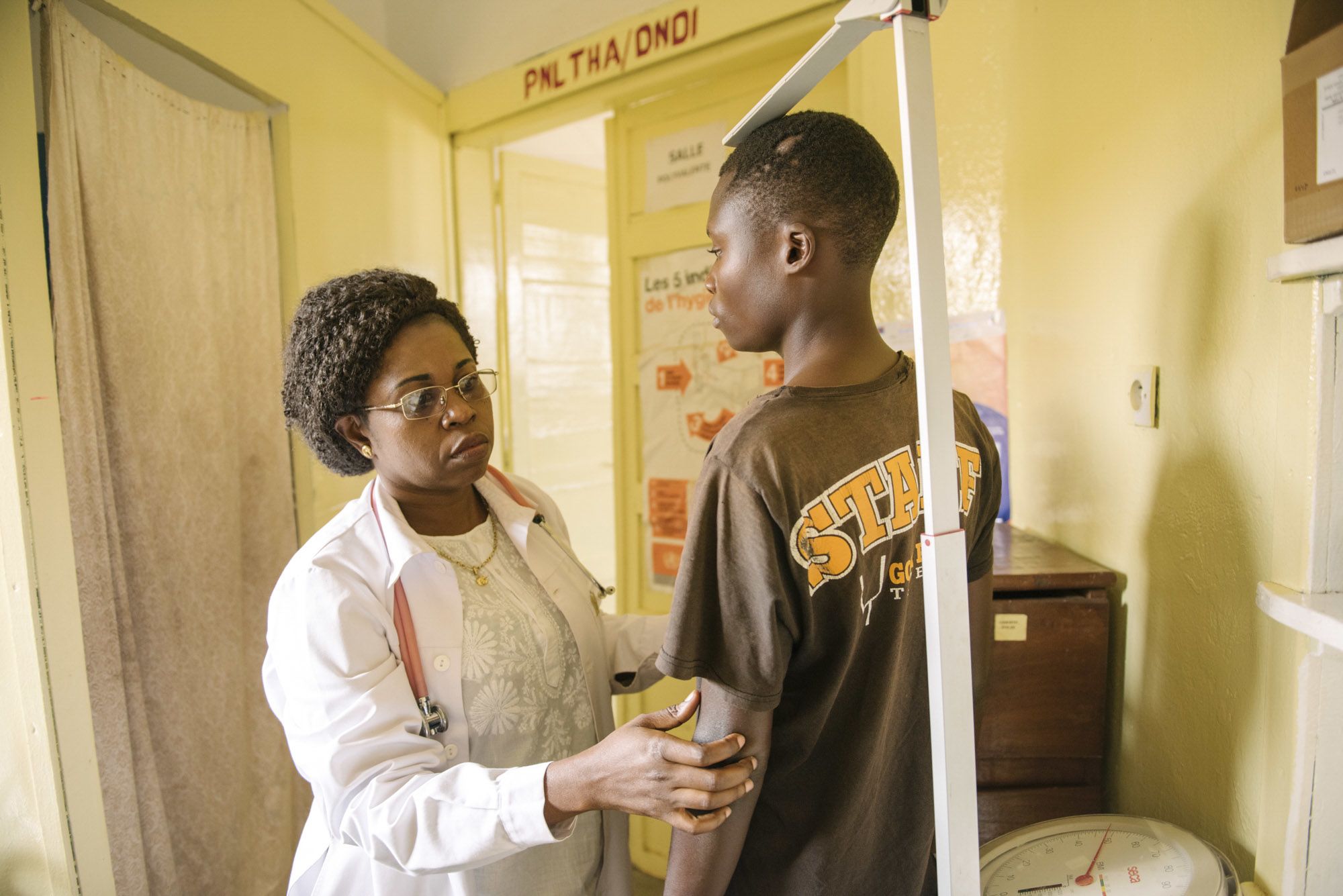
Dr Hélène analyzes Jonathan
Dr Hélène analyzes Jonathan
This is her first child to get sleeping sickness. “He has been sick for seven months – he sleeps a lot, gets angry – he even hits his friends,” she said. “He stopped working in the classroom and he stopped showing respect for his father and mother.”
“It is difficult to be here – my children are alone in the village now,” she adds.

Dr Hélène with NECT treatment for one patient
Dr Hélène with NECT treatment for one patient
Dr Hélène observes the treatment from afar. The sun has set and she is tired after a long day.
“NECT is extremely effective, but it's so hard to administer night and day – it's also hard for these families,” Dr Hélène says as her team administers the drugs. “Fexinidazole will be a great improvement.”

Dr Hélène standing outside the sleeping sickness ward, marked with a tsetse fly
Dr Hélène in her lab
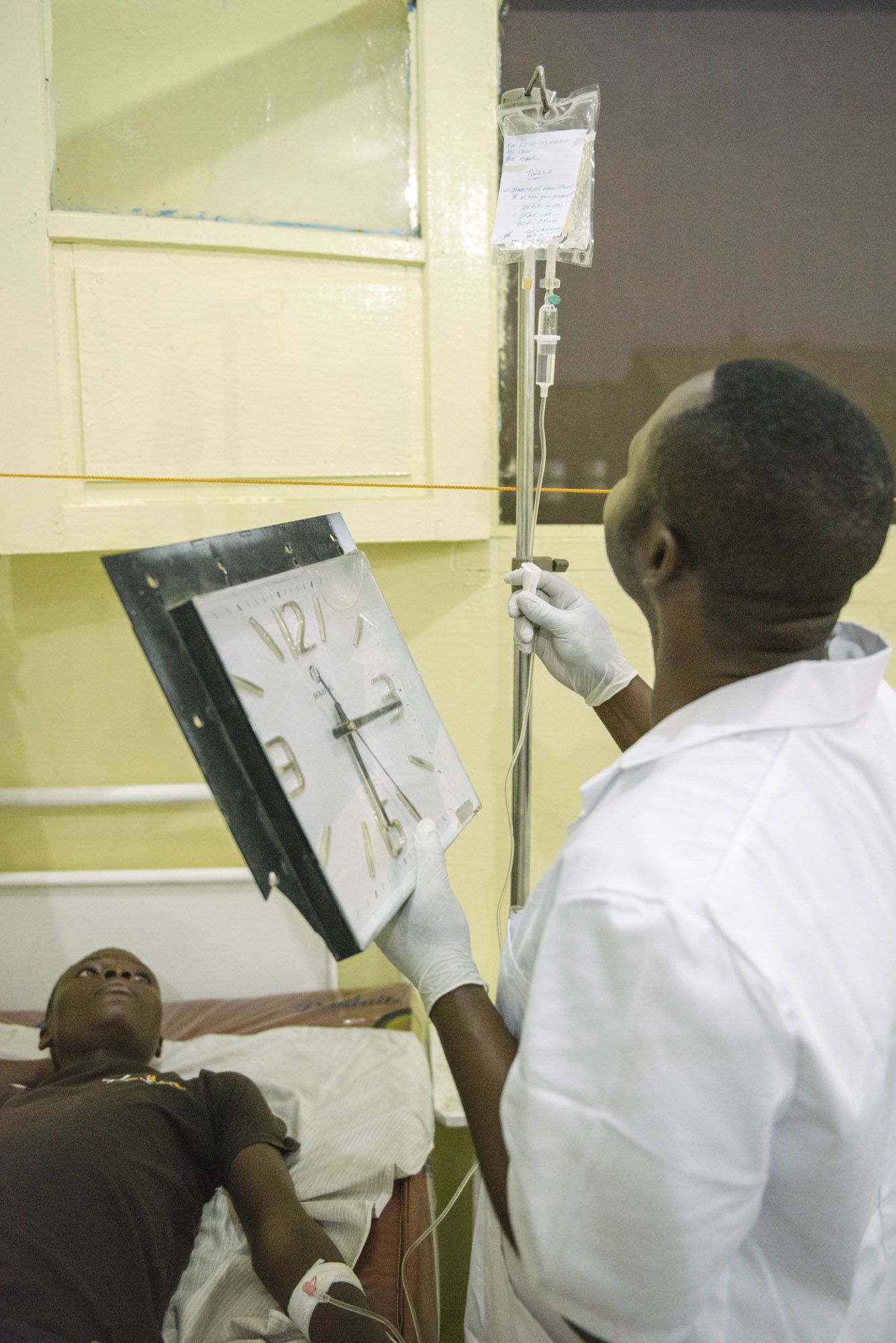
Infusions of NECT need to be timed - fexinidazole can be administred simply
Infusions of NECT need to be timed - fexinidazole can be administred simply

Mama Philomene
Mama Philomene
DNDi's clinical trials were conducted in 10 sites in the DRC and Central African Republic
Over 740 patients were recruited

DNDi-supported mobile teams screened over 2 million people in the DRC for sleeping sickness
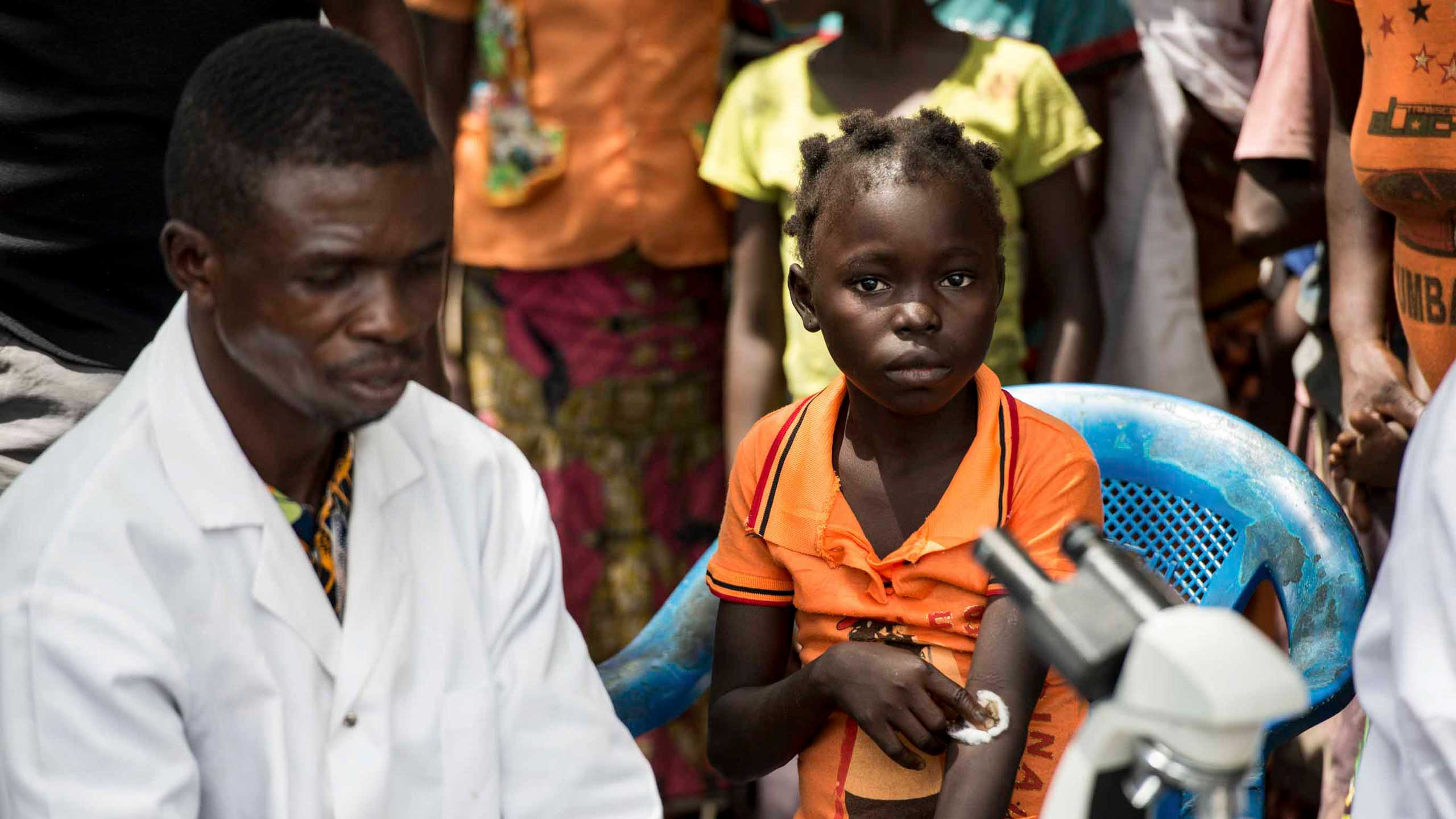

Genese Luyantiku Sindani is a farmer, 38 years old with four children – two boys and two girls. She lives in Masi Manimba. She is gentle but turns morose when she talks about beating her kids when she was suffering from sleeping sickness.
In 2011 she fell ill. She had headaches, backaches and fever. “I started hitting my children and I couldn’t control it," she said.
That being said, she has a hazy memory of those times. She went to the Masi Manimba hospital for her treatment: “The doctors did blood tests and a spinal tap, which hurt a lot.” She was enrolled in the fexinidazole clinical trials. “I am cured now,” she said.
“Genese was able to have two children after her treatment,” said Dr Willy. “This is important, because sleeping sickness can cause infertility and sterility in women of child-bearing age.”

Dr Willy with Genese
Dr Willy with Genese

François Ndona, 18, carries his bible with him wherever he goes.
He lives in Masi Manimba, and is a sleeping sickness survivor. In 2012 he was tested positive when a mobile team came to his school. He remembers: “I was always agitated. I always wanted to fight with other children and ended up getting into fights at school. At home, I was always angry.” '
He was at secondary school. “I had headaches and swollen glands.” He was punished at school for fighting.
He was treated in 2012 with fexinidazole in the clinical trials. “I no longer pick fights, I no longer feel like I used to when I had sleeping sickness.” He is now studying to enter into construction.


Back in Bagata, Dr Kande makes his way down the open-air walkways of the colonial-era hospital. Everything is bathed in the magnificent orange glow of the setting Congolese sun. Fishermen standing in narrow pirogue set off for the night on the Kwilu river below the hospital. It is calm.
When the doctor reaches the sleeping sickness ward and DNDi site, he slowly surveys the scene.

What a few decades ago was a jam-packed ward is now an orderly clinical site. Microscopes, computers, solar panels have replaced the boxes of toxic treatments. The beds – once packed with patients hooked up to IVs, their families surrounding them – are now empty.
To any casual visitor, it would be hard to imagine the countless stories of suffering that took place in this ward.
But not for Dr Kande. He – like so many Congolese doctors who have dedicated their lives to fighting the disease – has learned one thing from the peaks and valleys of sleeping sickness cases over the past century.
The disease can strike back.
"We have come so far in only a decade - from a treatment that killed patients, to a simple pill now," says Dr Kande. "We don't want to lose all the progress we made. Hopefully fexinidazole will help spell the end of this terrible cycle."
Dr Kande gets into his sturdy land cruiser, emblazoned with DNDi and MSF logos, and rides into the pitch black Congolese night onto the next clinical site.
A doctor's dream
For more information on fexinidazole and sleeping sickness, please click here

Photos by Xavier Vahed and Neil Brandvold
#sleepingsickness

THANK YOU TO OUR:
DONORS
Bill & Melinda Gates Foundation, USA; UK aid, UK; Dutch Ministry of Foreign Affairs (DGIS), The Netherlands; Federal Ministry of Education and Research (BMBF) through KfW, Germany; French Development Agency (AFD), France; German Corporation for International Cooperation (GIZ) on behalf of the Government of the Federal Republic of Germany, Germany; Ministry for Europe and Foreign Affairs, France, Médecins sans Frontières; Norwegian Agency for Development Cooperation (Norad), Norway; Republic and Canton of Geneva, Internal Solidarity Service, Switzerland; Spanish Agency for International Development and Cooperation (AECID), Spain; Swiss Agency for Development and Cooperation (SDC), Switzerland; UBS Optimus Foundation, Switzerland; Brian Mercer Charitable Trust, UK; Stavros Niarchos Foundation, USA and other private foundations and individuals from the HAT campaign.
PARTNERS
Accelera, Italy; Amatsi Aquitaine (formerly Bertin Pharma), France; Aptuit, Italy; BaseCon A/S, Denmark; Biotrial, France; Bruno Scherrer, France; Cardiabase, France; CBCO, DRC; Centipharm, France; Drugabilis, France; Institute of Tropical Medicine Antwerp, Belgium; Institut de Recherche pour le Développement, France; Institut National de Recherche Biomédicale, DRC; HAT Platform; Médecins Sans Frontières; National Control Programmes of the Democratic Republic of Congo, the Central African Republic, and Guinea; Phinc, France; Sanofi, France; SGS, Belgium; SGS, France; Swiss Tropical and Public Health Institute, Switzerland; WHO NTD Department, Switzerland.

